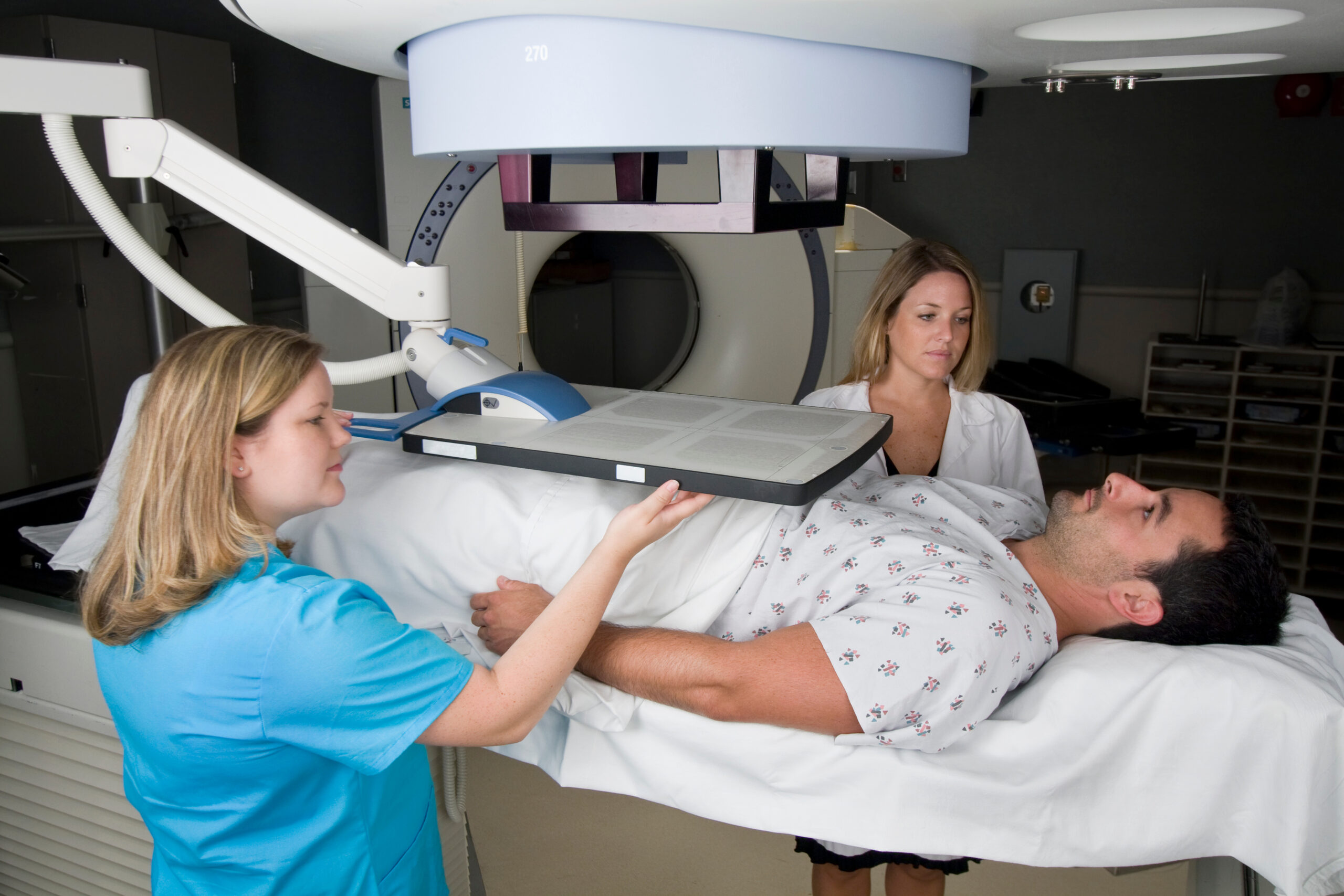
Radiation Therapy
Radiation therapy uses beams of high-energy radiation (photons) to kill cancer cells. Radiation damages the cancer cells’ DNA (the genetic material of the cancer cell), ultimately causing them to die. Healthy cells are also exposed to radiation, but they are able to repair their DNA, and so are less affected. Radiation therapy is very effective at killing localized prostate cancer and has the same cure rate as surgery.
With radiation therapy, the entire prostate gland is treated. Modern technology has evolved to minimize damage to surrounding non-cancerous cells; this is important because the prostate lies near the bladder and the rectum. Still, some normal tissue may be affected, causing side effects. Just as surgical skill can play an important role in determining outcomes from surgery, the technical skill of your radiation oncologist can affect your radiation therapy outcomes. If possible, choose a radiation oncologist with expertise in treating prostate cancer.
There are two main types of radiation therapy: External beam radiation therapy (EBRT) and brachytherapy.
External Beam Radiation Therapy (EBRT)
EBRT is the most common type of radiation therapy. This is when the radiation comes from the outside of the body.
What happens during EBRT?
Your doctor will do a “mapping” scan to precisely locate your prostate, rectum, and bladder, and use this information to design a personalized radiation therapy plan. Some physicians use gold markers or electromagnetic beacons that track the position of the prostate gland.
Radiation therapy is done on an outpatient basis over time (between 5 and 45 days – see Durations section below). You will come to the treatment center daily, and each appointment typically lasts less than an hour. The radiation is non-invasive, and you will not feel pain during the treatment.
You may experience some fatigue and/or have mild increased frequency of urination or bowel movements during the weeks of treatment. For more information, see Side Effects below. For men with higher-risk prostate cancer, radiation therapy is often combined with hormone therapy.
EBRT Treatment Durations
There are 3 treatment durations (number of treatments) that are used in EBRT. These are simply different schedules; all are effective in treating prostate cancer, but may have some different side effect profiles. Ask your doctor which option(s) are best for you.
Conventional: Patients come to the treatment center each weekday, for a total of 40–45 treatments over 8–9 weeks. This method has become less common.
Moderate hypofractionation: Radiation therapy is delivered in 20–28 treatments over 4–6 weeks. This is considered by national guidelines to be the current standard of care for many patients with localized prostate cancer.
Ultra-hypofractionation: Also known as stereotactic body radiation therapy (SBRT), this approach is delivered in about 5 treatments, using higher doses per day than moderate hypofractionation. This strategy is rapidly becoming more common because it may have equal cure rates, similar side effects and increased convenience. At many centers of excellence this is the standard of care. However, not all centers can safely provide this treatment, and not all patients are good candidates, so make sure to consult your doctor.
Brachytherapy
Brachytherapy involves a minimally-invasive procedure under anesthesia to place radiation therapy “seeds” inside the prostate. The seeds give off high doses of radiation to the area immediately around them, thus killing the prostate cancer cells. Think of it as internal radiation therapy, rather than external radiation therapy. There are two ways of delivering brachytherapy. One is called low dose rate, or LDR brachytherapy, in which the seeds are permanently implanted in the prostate. Over weeks to months, the radiation decays away and the seeds that remain are harmless.
The second type of brachytherapy is a high dose rate, or HDR brachytherapy. This involves inserting catheters into the prostate and temporarily placing seeds for a fixed period of time. The seeds are retracted and when the patient leaves, they don’t have anything radioactive left in their body.
Brachytherapy by itself is usually used only for low-risk or favorable intermediate-risk patients.
It can be used in combination with EBRT in intermediate- or high-risk patients. The success of brachytherapy, like surgery or EBRT, is dependent on the skill of your practitioner. Ask your doctor to help you find an experienced radiation oncology team who can perform brachytherapy.
Brachytherapy is less common than it used to be. Some patients prefer it because it doesn’t require daily visits to the treatment center. Brachytherapy may have increased urinary side effects compared to EBRT. Ask your doctor about safety precautions after the procedure, such as those pertaining to sexual activity and holding children in your lap (specifically for LDR brachytherapy).
If you are considering radiation therapy, ask your doctor about the benefits, risks, and logistics involved with each type.
Side Effects
Radiation therapy has some possible side effects to be aware of. Dr. George Zhao discusses these in the video below.