PSMA PET Imaging – What it Is and How it Helps Guide Your Care
What is a PSMA PET scan?
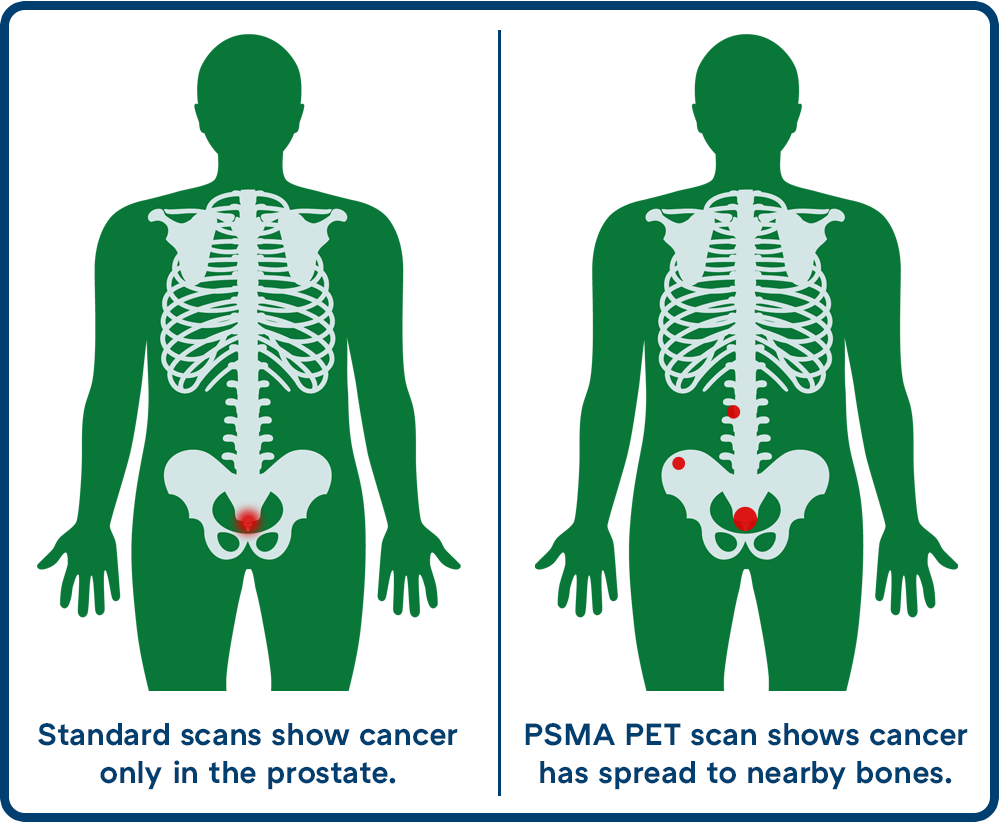
PSMA PET is an advanced, highly sensitive, whole-body imaging scan that helps find even very small areas of prostate cancer, which standard scans often miss.
This scan can give a clearer picture of any prostate cancer that has spread in your body. This helps you get the right treatment.
The letters stand for:
- PSMA – Prostate-Specific Membrane Antigen, a protein found in large amounts on most prostate cancer cells. Not the same as PSA.
- PET – Positron Emission Tomography, the technology used to take the images.
Who Should Consider This Scan?
Your doctor may suggest a PSMA PET scan if:
- You were recently diagnosed and are thinking about getting surgery or radiation. PSMA PET helps show if cancer has spread outside your prostate. This helps you and your doctor plan the right treatment.
- Your PSA is rising after treatment. A rising PSA can mean the cancer has come back somewhere in your body – PSMA PET can help find where.
- You have advanced prostate cancer. PSMA PET helps show if you may benefit from radioligand therapy, a targeted treatment that finds prostate cancer cells and directly delivers radiation to damage and kill them.
How Does a PSMA PET Scan Work?
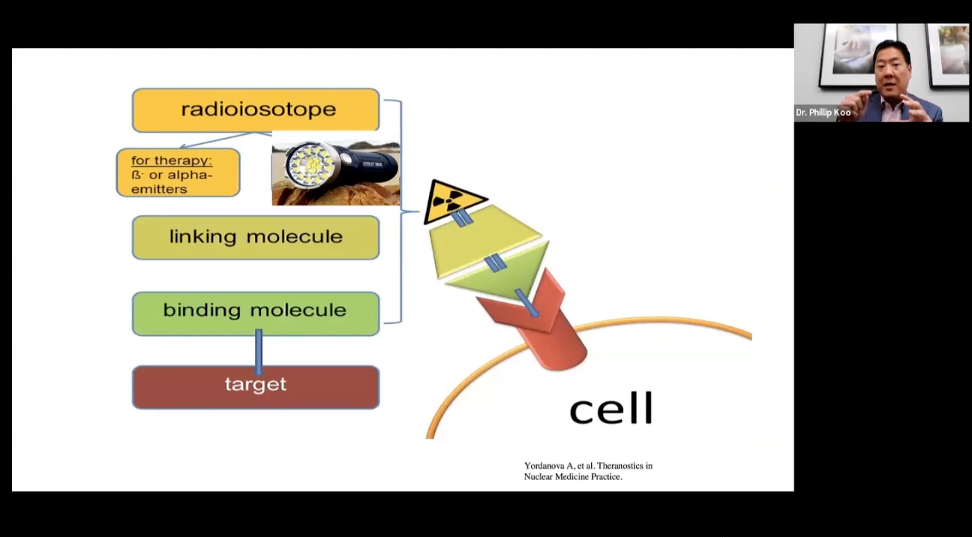
Before the scan, you get a shot through an IV. The injection contains a special imaging agent that has:
- A tracer that travels through your body and attaches to the PSMA protein on prostate cancer cells.
- A small radiation source, or radioisotope, which the PET camera can detect.
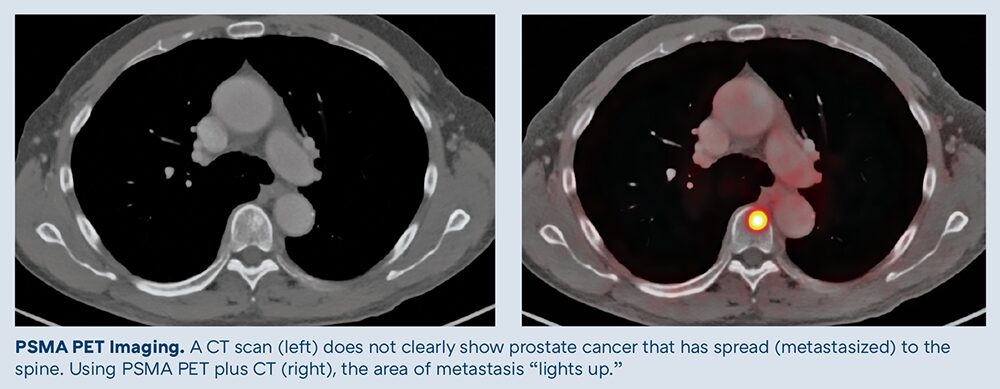
After the tracer attaches to prostate cancer cells, areas of prostate cancer show up as bright spots on the scan.
The scan typically takes up to 30 minutes. You will wait for the imaging agent to move through your body and then lie on a table while the scanner takes pictures. A CT scan is done at the same time to show exactly where any bright spots are in your body.
What Do the Results of PSMA PET Mean for My Treatment?
A PSMA PET scan gives your care team a detailed ‘map’ of where prostate cancer is — and isn’t — in your body, so you can plan the best treatment.
- If you are newly diagnosed: If the scan shows no cancer outside your prostate, surgery or radiation therapy is more likely to work well. If the scan does find cancer outside the prostate, your treatment plan can be adjusted.
- If you already had treatment and your PSA is rising: A PSMA PET scan can help show where the cancer has come back – in the prostate, pelvis, or somewhere else. This helps guide next steps.
- If you have advanced prostate cancer: The scan helps find the cancer and shows if it has enough PSMA for radioligand therapy to find and target it.
Is the Radiation Safe?
Like all imaging scans, PSMA PET uses a small amount of radiation. Your doctor will recommend the scan if the benefits for you are expected to outweigh any risks.
Most people can go back to their usual activities right after a PSMA PET scan. Your doctor may ask you to drink more fluids for a day or two to help clear the tracer from your body. Allergic reactions to the imaging agent are rare.
What Else Should I Know?
PSMA PET only finds prostate cancer that makes the PSMA protein. Most prostate cancers make PSMA, but not all.
The scan also works better when PSA is higher. Your doctor may ask to wait to order a scan until your PSA reaches a certain level.
Very small clusters of prostate cancer cells may not show up on a scan. This means that lymph nodes removed during surgery sometimes contain prostate cancer cells even though your PSMA PET scan was negative.
Some normal tissues also make PSMA. Your doctor will look closely at any bright spots to decide if they are likely to be prostate cancer.
Last Reviewed: 05/2026