What are somatic
and germline
genetic testing?
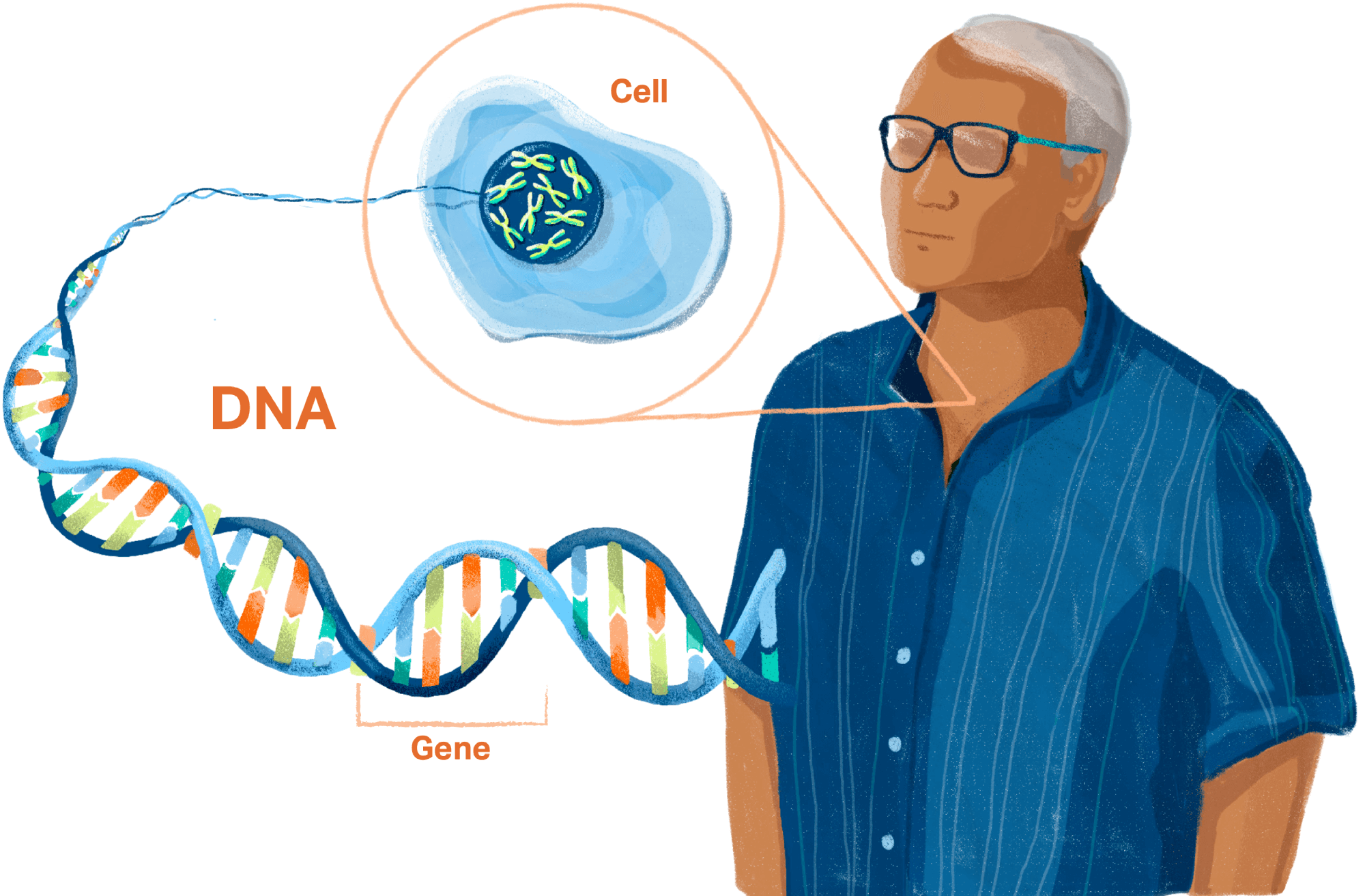
If you have advanced prostate cancer, there are two types of genetic tests (somatic and germline) that are important to help guide your treatment choice.
How can these
tests help me?
Getting both somatic and germline genetic testing will give you and your doctor the most complete understanding of your treatment options.

Understanding
your test results.
Understanding the basics of your test reports will help you ask questions and talk to your doctor.

Talking with
your doctor.
It’s a good idea to ask about somatic and germline genetic testing during your appointments.


Get the Patient Guide

